Trigger Finger
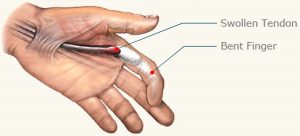 Trigger finger is a condition in which one of your fingers gets stuck in a bent position. Your finger may bend or straighten with a snap — like a trigger being pulled and released.
Trigger finger is a condition in which one of your fingers gets stuck in a bent position. Your finger may bend or straighten with a snap — like a trigger being pulled and released.
Tendons are fibrous cords that attach muscle to bone. Each tendon is surrounded by a protective sheath. Trigger finger occurs when the affected finger’s tendon sheath becomes irritated and inflamed. This interferes with the normal gliding motion of the tendon through the sheath. Prolonged irritation of the tendon sheath can produce scarring, thickening and the formation of bumps (nodules) in the tendon that impede the tendon’s motion even more.
People with work or hobbies that require repetitive gripping actions are at higher risk of developing trigger finger. The condition is also more common in women and people who suffer with diabetes.
Symptoms
Signs and symptoms of trigger finger may progress from mild to severe and include:
- Finger stiffness, particularly in the morning
- A popping or clicking sensation as you move your finger
- Tenderness or a bump (nodule) on palmside at the base of the affected finger
- Finger catching or locking in a bent position, which suddenly pops straight
- Finger locked in a bent position, which you are unable to straighten
Trigger finger can affect any finger and triggering is usually more pronounced in the morning.
Diagnosis
Diagnosis of trigger finger doesn’t require any elaborate testing. Diagnosis is based on medical history and a physical exam. During the physical exam, your doctor/physo will ask you to open and close your hand, checking for areas of pain, smoothness of motion and evidence of locking. He should also feel your palm to see if there is a lump present. If the lump is associated with trigger finger, the lump will move as the finger moves because the lump is an area of swelling in part of the tendon that moves the finger.
Treatment
Trigger finger treatment varies depending on the severity and duration of the condition. Nonsteroidal anti-inflammatory drugs may relieve the pain but are unlikely to relieve the swelling constricting the tendon sheath or trapping the tendon.
Conservative non-invasive treatments may include:
- Rest. Avoid activities that require repetitive gripping, repeated grasping or the prolonged use of vibrating hand-held machinery until your symptoms improve. If you can’t avoid these activities altogether, padded gloves may offer some protection.
- A splint. Your doctor may have you wear a splint at night to keep the affected finger in an extended position for up to six weeks. The splint helps rest the tendon.
- Stretching exercises. Your doctor may also suggest gentle exercises to help maintain mobility in your finger.
If conservative treatment fails here are the other options.
- Steroid injection. Injection of a steroid medication near to or into the tendon sheath may reduce inflammation and allow the tendon to glide freely again. This is the most common treatment, and it’s usually effective for a year or more in most people treated. Sometimes it takes more than one injection. For people with diabetes, steroid injections tend to be less effective.
- Percutaneous release. After numbing your palm/finger, your doctor inserts a sturdy needle into the tissue around your affected tendon. Moving the needle and your finger helps break apart the constriction that is blocking the smooth motion of the tendon.This treatment may be done under ultrasound control, so the doctor can see where the tip of the needle is under the skin and to be sure it opens the tendon sheath without damaging the tendon or nearby nerves.
- Surgery. Working through a small incision near the base of your affected finger, a surgeon can cut open the constricted section of tendon sheath. This is a last resort.
Update
Here is a video of exercises to get rid of trigger finger, I came across by the internet famous physical therapists Bob and Brad. These exercises have actually proved to be extremely effective …….See video
Physio in Tralee phone 086-7700191
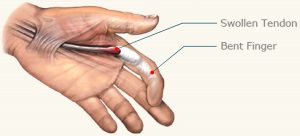
 Trigger finger is a condition in which one of your fingers gets stuck in a bent position. Your finger may bend or straighten with a snap — like a trigger being pulled and released.
Trigger finger is a condition in which one of your fingers gets stuck in a bent position. Your finger may bend or straighten with a snap — like a trigger being pulled and released.