Common Knee Injuries
1. Chondromalacia Patella
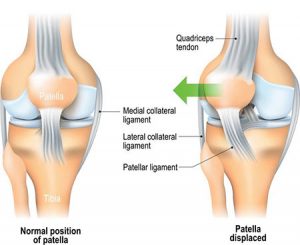 Knee injuries like Chondromalacia patella result from degeneration of cartilage on the underside the kneecap (patella)due to poor alignment of the kneecap (patella) as it slides over the lower end of the thighbone (femur). This condition can also be referred to as patellofemoral syndrome. It usually presents as pain in the front of the knee aggravated by activities such as running, jumping, climbing or descending stairs etc., or by prolonged sitting with knees in a moderately bent position. Patients with chondromalacia patella frequently have abnormal patellar “tracking” toward the lateral (outer) side of the femur. Some patients may also have a vague sense of “tightness” or “fullness” in the knee area with the condition. Mild swelling of the knee area may also occur.
Knee injuries like Chondromalacia patella result from degeneration of cartilage on the underside the kneecap (patella)due to poor alignment of the kneecap (patella) as it slides over the lower end of the thighbone (femur). This condition can also be referred to as patellofemoral syndrome. It usually presents as pain in the front of the knee aggravated by activities such as running, jumping, climbing or descending stairs etc., or by prolonged sitting with knees in a moderately bent position. Patients with chondromalacia patella frequently have abnormal patellar “tracking” toward the lateral (outer) side of the femur. Some patients may also have a vague sense of “tightness” or “fullness” in the knee area with the condition. Mild swelling of the knee area may also occur.
2. Meniscus Tear – Knee injuries
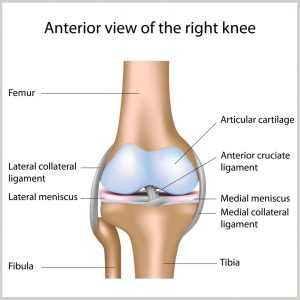 Any activity that causes you to forcefully twist or rotate your knee, especially when putting your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You might also feel your knee lock and have trouble extending it fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and allow the injury time to settle down on its own. In other cases, however, a torn meniscus requires surgical repair.
Any activity that causes you to forcefully twist or rotate your knee, especially when putting your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You might also feel your knee lock and have trouble extending it fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and allow the injury time to settle down on its own. In other cases, however, a torn meniscus requires surgical repair.
The meniscus weakens with age. Tears are more common in people over the age of 30. If you have osteoarthritis, you’re at higher risk of injuring your knee or tearing your meniscus. When an older person experiences a meniscus tear, it’s more likely to be related to degeneration. This is when the cartilage in the knee becomes weaker and thinner.
3. Cruciate ligament rupture
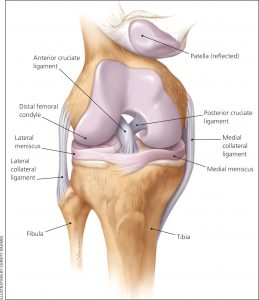 These ligaments are found inside your knee joint. They cross each other to form an “X” with the anterior cruciate ligament in front and the posterior cruciate ligament in back. The cruciate ligaments stabilize the knee. About half of all injuries to the anterior cruciate ligament occur along with damage to other structures of the knee, such as articular cartilage, meniscus, or other ligaments. Partial tears of the anterior cruciate ligament are rare; most ACL injuries are complete or near complete tears.
These ligaments are found inside your knee joint. They cross each other to form an “X” with the anterior cruciate ligament in front and the posterior cruciate ligament in back. The cruciate ligaments stabilize the knee. About half of all injuries to the anterior cruciate ligament occur along with damage to other structures of the knee, such as articular cartilage, meniscus, or other ligaments. Partial tears of the anterior cruciate ligament are rare; most ACL injuries are complete or near complete tears.
The cruciate ligaments can be injured in several ways such as : changing direction rapidly ; Stopping suddenly ; Slowing down while running ; Landing from a jump incorrectly ; Direct contact or collision to the knee.
When you tear a cruciate ligament, you might hear a “popping” noise and you may feel your knee give way under you. Other typical symptoms include:
- Pain with swelling. Within 24 hours, your knee will swell. If ignored, the swelling and pain may resolve on its own. However, if you attempt to return to sports, your knee will probably be unstable and you risk causing further damage to the cushioning cartilage (meniscus) of your knee.
- Loss of full range of motion
- Tenderness along the joint line
- Discomfort while walking
Treatment for a cruciate ligament tear varies depending on the patient’s individual needs. For example, the young athlete involved in agility sports will need surgery to return safely to sports. Less active, older individuals may be able to return to a quieter lifestyle without surgery.
4. Collateral ligament strain/rupture – Knee injuries
 The collateral ligaments of the knee are located one on either side of your knee joint. They help connect the bones of your upper and lower leg, inside your knee joint. The collateral ligaments help keep your knee stable. They keep your leg bones in place and keep your knee from moving too far sideways. A collateral ligament injury occurs when the ligaments are stretched or torn. A partial tear occurs when only part of the ligament is torn. A complete tear occurs when the entire ligament is torn into two pieces. A collateral ligament injury can occur if you get hit very hard on the inside or outside of your knee, or when you have a twisting injury. Sometimes the ligaments just sprain and this is easier to recover from and requires no surgery.
The collateral ligaments of the knee are located one on either side of your knee joint. They help connect the bones of your upper and lower leg, inside your knee joint. The collateral ligaments help keep your knee stable. They keep your leg bones in place and keep your knee from moving too far sideways. A collateral ligament injury occurs when the ligaments are stretched or torn. A partial tear occurs when only part of the ligament is torn. A complete tear occurs when the entire ligament is torn into two pieces. A collateral ligament injury can occur if you get hit very hard on the inside or outside of your knee, or when you have a twisting injury. Sometimes the ligaments just sprain and this is easier to recover from and requires no surgery.
With a collateral ligament injury, you may notice:
- Your knee is unstable and can shift side to side as if it “gives way”
- Locking or catching of the knee with movement
- Knee swelling
- Knee pain along the inside or outside of your knee
Various orthopedic tests can help diagnose collateral ligament damage. More detailed knowledge of the injury can be obtained by MRI. Injured ligaments are considered “sprains” and are graded on a severity scale.
If you have a collateral ligament injury, you may need:
- Crutches to walk until the swelling and pain get better
- A brace to support and stabilize your knee
- Physical therapy to help improve joint motion and leg strength
A lot of the time people don’t need surgery for collateral ligament damage but more serious cases may.
5. Baker’s Cyst – Knee injuries
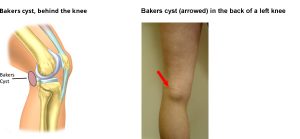
Baker’s cyst is a fluid-filled swelling that causes a lump at the back of the knee, leading to tightness and restricted movement. Usually, this condition is due to an underlying problem affecting the knee joint, such as arthritis or a cartilage injury.
6. Patella Tendinopathy
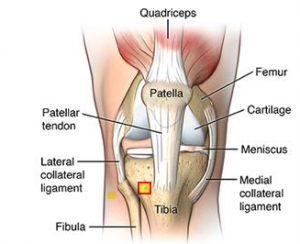 Patellar tendinopathy(also known as Jumper’s knee) is an overuse injury affecting this knee tendon. There are a number of factors which can contribute to the development of patellar tendinopathies. These include:
Patellar tendinopathy(also known as Jumper’s knee) is an overuse injury affecting this knee tendon. There are a number of factors which can contribute to the development of patellar tendinopathies. These include:
- Rapid increase in amount of training
- Sudden increase in training intensity
- Playing/training on rigid surfaces
- Tight quadriceps and hamstring muscles
- Poor foot posture, knee or hip control.
Tendinopathies usually causes pain, stiffness, and loss of strength in the affected area. The pain may get worse when you use the tendon. An experienced practitioner will be able to diagnose a tendinopathy from both palpation and history of the condition. Tendinopathies can be confirmed by MRI which will give a clearer picture of the level of damage. Treatment for patellar tendinopathies varies depending on the level of injury and can vary from conservative treatment combining rest / eccentric training to surgical intervention in more serious cases.
7. Osgood Schlatter’s Disease(Kids)
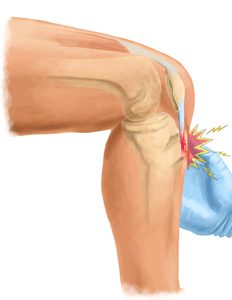 Osgood-Schlatter disease is a common cause of knee pain in growing adolescents. It is an inflammation of the area just below the knee where the tendon from the kneecap (patellar tendon) attaches to the shinbone (tibia) called the tibial tuberosity. The condition gets worse with activity and better with rest. Osgood-Schlatter disease most often occurs during growth spurts, when bones, muscles, tendons, and other structures are changing rapidly. Because physical activity puts additional stress on bones and muscles, children who participate in athletics — especially running and jumping sports – are at an increased risk for this condition. However, less active adolescents may also experience this problem. The condition normally resolves over time but can be anything from a few weeks/months to two years. It is nothing to worry about. A child can remain active but pain from the condition itself will limit that activity. Icing the area of pain and stretching leg muscles especially quads can help. NSAIDs can be used to relief the pain and inflammation but should be used sparingly and under doctors supervision.
Osgood-Schlatter disease is a common cause of knee pain in growing adolescents. It is an inflammation of the area just below the knee where the tendon from the kneecap (patellar tendon) attaches to the shinbone (tibia) called the tibial tuberosity. The condition gets worse with activity and better with rest. Osgood-Schlatter disease most often occurs during growth spurts, when bones, muscles, tendons, and other structures are changing rapidly. Because physical activity puts additional stress on bones and muscles, children who participate in athletics — especially running and jumping sports – are at an increased risk for this condition. However, less active adolescents may also experience this problem. The condition normally resolves over time but can be anything from a few weeks/months to two years. It is nothing to worry about. A child can remain active but pain from the condition itself will limit that activity. Icing the area of pain and stretching leg muscles especially quads can help. NSAIDs can be used to relief the pain and inflammation but should be used sparingly and under doctors supervision.
Article by Eddie O Grady Physiotherapist.
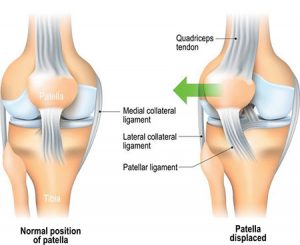
 Knee injuries like Chondromalacia patella result from degeneration of cartilage on the underside the kneecap (patella)due to poor alignment of the kneecap (patella) as it slides over the lower end of the thighbone (femur). This condition can also be referred to as patellofemoral syndrome. It usually presents as pain in the front of the knee aggravated by activities such as running, jumping, climbing or descending stairs etc., or by prolonged sitting with knees in a moderately bent position. Patients with chondromalacia patella frequently have abnormal patellar “tracking” toward the lateral (outer) side of the femur. Some patients may also have a vague sense of “tightness” or “fullness” in the knee area with the condition. Mild swelling of the knee area may also occur.
Knee injuries like Chondromalacia patella result from degeneration of cartilage on the underside the kneecap (patella)due to poor alignment of the kneecap (patella) as it slides over the lower end of the thighbone (femur). This condition can also be referred to as patellofemoral syndrome. It usually presents as pain in the front of the knee aggravated by activities such as running, jumping, climbing or descending stairs etc., or by prolonged sitting with knees in a moderately bent position. Patients with chondromalacia patella frequently have abnormal patellar “tracking” toward the lateral (outer) side of the femur. Some patients may also have a vague sense of “tightness” or “fullness” in the knee area with the condition. Mild swelling of the knee area may also occur. Any activity that causes you to forcefully twist or rotate your knee, especially when putting your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You might also feel your knee lock and have trouble extending it fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and allow the injury time to settle down on its own. In other cases, however, a torn meniscus requires surgical repair.
Any activity that causes you to forcefully twist or rotate your knee, especially when putting your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You might also feel your knee lock and have trouble extending it fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and allow the injury time to settle down on its own. In other cases, however, a torn meniscus requires surgical repair. These ligaments are found inside your knee joint. They cross each other to form an “X” with the anterior cruciate ligament in front and the posterior cruciate ligament in back. The cruciate ligaments stabilize the knee. About half of all injuries to the anterior cruciate ligament occur along with damage to other structures of the knee, such as articular cartilage, meniscus, or other ligaments. Partial tears of the anterior cruciate ligament are rare; most ACL injuries are complete or near complete tears.
These ligaments are found inside your knee joint. They cross each other to form an “X” with the anterior cruciate ligament in front and the posterior cruciate ligament in back. The cruciate ligaments stabilize the knee. About half of all injuries to the anterior cruciate ligament occur along with damage to other structures of the knee, such as articular cartilage, meniscus, or other ligaments. Partial tears of the anterior cruciate ligament are rare; most ACL injuries are complete or near complete tears.
 Patellar tendinopathy(also known as Jumper’s knee) is an overuse injury affecting this knee tendon. There are a number of factors which can contribute to the development of patellar tendinopathies. These include:
Patellar tendinopathy(also known as Jumper’s knee) is an overuse injury affecting this knee tendon. There are a number of factors which can contribute to the development of patellar tendinopathies. These include: Osgood-Schlatter disease is a common cause of knee pain in growing adolescents. It is an inflammation of the area just below the knee where the tendon from the kneecap (patellar tendon) attaches to the shinbone (tibia) called the tibial tuberosity. The condition gets worse with activity and better with rest. Osgood-Schlatter disease most often occurs during growth spurts, when bones, muscles, tendons, and other structures are changing rapidly. Because physical activity puts additional stress on bones and muscles, children who participate in athletics — especially running and jumping sports – are at an increased risk for this condition. However, less active adolescents may also experience this problem. The condition normally resolves over time but can be anything from a few weeks/months to two years. It is nothing to worry about. A child can remain active but pain from the condition itself will limit that activity. Icing the area of pain and stretching leg muscles especially quads can help. NSAIDs can be used to relief the pain and inflammation but should be used sparingly and under doctors supervision.
Osgood-Schlatter disease is a common cause of knee pain in growing adolescents. It is an inflammation of the area just below the knee where the tendon from the kneecap (patellar tendon) attaches to the shinbone (tibia) called the tibial tuberosity. The condition gets worse with activity and better with rest. Osgood-Schlatter disease most often occurs during growth spurts, when bones, muscles, tendons, and other structures are changing rapidly. Because physical activity puts additional stress on bones and muscles, children who participate in athletics — especially running and jumping sports – are at an increased risk for this condition. However, less active adolescents may also experience this problem. The condition normally resolves over time but can be anything from a few weeks/months to two years. It is nothing to worry about. A child can remain active but pain from the condition itself will limit that activity. Icing the area of pain and stretching leg muscles especially quads can help. NSAIDs can be used to relief the pain and inflammation but should be used sparingly and under doctors supervision.